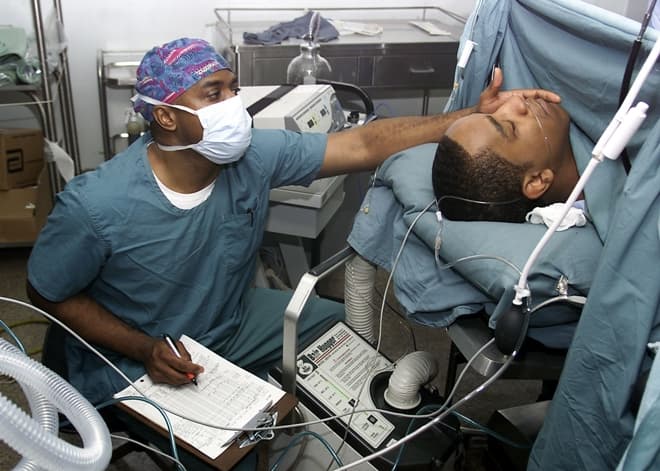
Photo Credit: by U.S. Navy photo / Wikimedia Commons
Besides eliciting the occasional jab in the ribs from a sleeping partner, heavy snoring is a seemingly benign phenomenon. But snoring in fact could indicate the presence of one sleeping giant of an issue when it comes to post-operative healing: OSA, otherwise known as obstructive sleep apnea. Individuals afflicted with this disorder after surgery face more post-operative complications and a much longer recovery time before they are finally able to rise from their hospital beds and emerge into the outdoor air.
Apart from the 5.4 million Canadians who have received a diagnosis of OSA there are many who unknowingly live with this disorder. For a doctor to implement the proper procedures, to avoid post-operative complications, it is imperative to be aware of whether a patient has OSA. People with OSA tend to snore heavily, be overweight, endure daytime sleepiness, experience morning headaches, and awaken throughout the night. These symptoms could be signs you have OSA—so it’s critical to get checked for the condition before undergoing surgery.
Physiologically speaking, the problems occur when airflow through the upper airway is repeatedly interrupted during sleep as the pharyngeal tissues at the back of the throat collapse, temporarily closing the airway. Compounded over an entire night’s sleep, this action results in serious decreases in bodily oxygen levels. An important thing to note is that the use of sleep medication or other sedatives before bedtime actually exacerbates this condition by relaxing the throat muscles even further and causing an increase in pharyngeal collapses throughout the night.
Even slight drop-offs in balanced oxygen levels in the blood can dramatically impact health. At sea level 96-97% would be considered normal, while long time sufferers of OSA would be in the low 90% range. A 5% decrease in blood oxygen could cause hypoxia and the concurrent medical complications. Recent studies on the link between oxygen deprivation in wound tissues and rates of healing have concluded that a lack of oxygen in wound tissues, known as hypoxia, results in a dramatically slower recovery, bouts of encephalopathy, and a lowered resistance against bacterial infections. The complications occur because oxygen plays such a major role in the metabolism of ATP, and also oxygen is a vital element in protein synthesis, angiogenesis (“the sprouting of blood vessels from existing vessels”), and cell proliferation, which are the processes that comprise the regeneration of bodily tissues.
As this knowledge has been absorbed by the medical community, doctors have become aware of the need to customize operative procedures to suit the requirements of patients. The first step in this includes a screening process to identify if the patient even has OSA, as often it is undiagnosed.
If the patient is found to have OSA then several courses of action can be taken. If the condition requires higher dosages of opioids, placement in a hospital unit with higher supervision and the ability to undergo oximetry would be highly beneficial to monitor healing progress and oxygen saturation levels in the blood.
After surgery, too, there are several options for those with OSA. One ground breaking therapy is HBOT-hyperbaric oxygen therapy. This therapy is commonly used for decompression sickness in scuba divers. Using the same principle, as an individual with OSA enters the hyperbaric oxygen chamber, the oxygen concentration in the air would be 3 times that of normal air. Breathing in this higher concentration of oxygen has been shown to significantly improve the wound healing in 90% of patients. It is less commonly used because of the risks associated with HBOT: middle ear injuries, near-sightedness, and in severe cases collapsed lungs or seizures.
CPAP, continuous positive airway pressure, is another effective technique. Through the use of a mask connected to a device, air pressure is increased in the throat to prevent the collapse of the airway during sleep.
Lastly, non-invasive, good old-fashioned breathing exercises could provide an answer. Much in the same fashion that push-ups train muscles, breathing techniques can increase the efficiency of the respiratory system and increase oxygen levels in the blood. In the field of Chinese medicine it is believed that the quality of breath is fundamentally tied to good health. As a result breathing techniques were studied for centuries and practiced to promote wellbeing. If practiced regularly in the months leading up to surgery, these techniques and modern oropharyngeal exercises could potentially have a positive impact on balancing oxygen blood saturation levels in OSA patients and minimize post-operative complications.
The results prove it: better breathing during sleep means better healing. Further studies will be able to provide the ideas and subsequent access to therapies that can alleviate the prolonged post-operative pain of those with obstructive sleep apnea.
###
Cody MacInnis is currently studying the connections between biological and mental processes in Victoria B.C. His free time is spent outside enjoying the fresh Vancouver Island air.
Your email address will not be published. Required fields are marked with *.